Personal trainers preach that healthy insides, accomplished through clean eating, lead to improved overall health. Now conclusive research points to how improving one’s diet may alter the intestinal microbiota, further promoting successful aging and optimal weight. This approach, manifested by a research consortium comprised of nutritionists, bio-gerontologists, immunologists, and molecular biologists, has become known as the Mediterranean, or NU-AGE, diet.
The Far-Reaching Effects of Gut Health and Bacteria
As the human body ages, inflammation often develops and flares up, along with the deterioration of multiple bodily systems, setting seniors up for frail golden years. Scientists now have reason to believe that certain aspects of what we call the “Standard American (or Western) Diet” or SAD, contribute to this condition, underscored by negative processes within the human gut. Characterized by decreased walking speed, weakened bones, diminished muscle strength, and low energy, frailty in the aging population heightens risk of accidental falls, fractures leading to disability, and an increased need for advanced nursing care facilities.
The Gut-Microbiome, Inflammation, and Obesity
Systemic chronic low-grade inflammation, often associated with obesity, renders an individual prone to cardiovascular diseases and type 2 diabetes. Past research honed in on unregulated adipose tissue or insulin resistance as the main culprits in inflammation. However, systemic inflammation involves a complexity only recently studied and is still somewhat of a mystery.
Chronic inflammation often presents in individuals consuming a high-fat diet; scientists now posit whether this condition appears as a prelude to obesity-related metabolic disorders, not an end product since the gut microbiome appears substantially different in those living with autoimmune diseases, obesity, and other metabolic disorders.
Considering the human gastrointestinal system receives first exposure to everything we ingest, the supposition exists that as diet affects the gut microflora, systemic inflammation might result. The medical community feels that a promising step rests on the premise that restoring gut microbiota composition (by dietary intervention, prebiotics, and probiotics) could mitigate disease.
The Science Confirms the Meal Plan Advantages
Knowing that poor nutrition can easily lead to detrimental health, researchers began to consider how different meal plans might positively influence geriatric frailty. Several studies looked at almost 6,000 volunteers from France, Spain, China, and Italy. Interestingly enough, data pointed to the virtues of the Mediterranean diet, according to an article published in the Journal of the American Geriatrics Society.
“We found the evidence was very consistent that older people who follow a Mediterranean diet had a lower risk of becoming frail,” said researcher Kate Walters, from the University College London. “People who followed a Mediterranean diet the most were overall less than half as likely to become frail over a nearly four-year period compared with those who followed it the least.”
The Mediterranean Menu
Indeed, individuals of Mediterranean descent following the eating habits of their ancestors show evidence of robust longevity. A Mediterranean diet extolls the virtues of meals based around whole, single-ingredient plant-sourced foods. Fresh and dried fruits, vegetables, legumes, whole grains, fresh fish, olive oil, and fermented dairy products comprise the backbone of this plan. Red meat, refined sugar, and processed foods rarely get consumed. Plenty of water and a daily glass of red wine figure prominently, along with reasonable amounts of physical activity and plenty of community socialization.
Bacterial Biodiversity and Weight Loss
Over a trillion species of bacteria and other microbes reside in the human digestive system, forming what medical professionals refer to as the gut microbiota. These “good” bacteria aid in breaking down food and also confer some disease protection. When the bacterial biodiversity gets thrown off-kilter from a lifetime of poor nutrition, the gut microbiota suffers, leading to an increase in frailty along with a host of other comorbid situations.
There likewise exists a strong association between a healthy gut microbiome and a lean body composition. Many of us grew up with the notion that weight loss came down to a simple matter of calories in versus calories out. While that may hold true, the complexity of the equation has recently piqued the interest of scientists. The burning question: Which kinds of calories promote the best chance of successful weight loss?
Processed versus High-Fiber Intake
Researchers have posed and pondered the issue of why calories from certain types of foods lead to sluggish or negligible weight loss, while other choices promote loss at a healthy rate.
As it turns out, the gut microbiome (the population of healthy working bacteria located near the end of the digestive tract) responds poorly to highly processed foods. Such food choices get rapidly absorbed within the upper GI tract, enabling more calories to linger in the body. Conversely, foods boasting a high fiber content foster a much slower absorption rate, thereby enabling them to actually reach the large intestine. There, the trillions of good bacteria lie, waiting to be fed and nurtured. The latest study shows that by “feeding” our intestinal microbes, we essentially reduce caloric intake.
Energy and Macro Balance
Scientists refer to the gut microbiome as a vital component in the balance of energy. Another study used a “Microbiome Enhancer Diet” (very similar to a Mediterranean diet) to feed one group of subjects, while the other group consumed a typical “Western diet” containing many processed food sources. Since the microbe-enhancing meal plan contained high-fiber and nutrient-dense foods, this group demonstrated approximately 116 more kcal eliminated in feces when compared to the Western diet group.
Another study was conducted with two groups of subjects: one received a high-fat diet, the other continued to consume normal meals. Data revealed that the higher fat diet aligned with significant changes in the gut microbiome, intestinal permeability, and systemic low-grade inflammation. Glucose tolerance also plummeted in the high-fat group.
Armed now with the strong conviction that one’s gut health and microbiome plays a key role in the appearance of inflammation and altered metabolic pathways, future studies plan to assess whether probiotics might serve as an important tool in both the treatment and prevention of obesity and Type 2 diabetes.
The significant difference in metabolizable energy within the body seems, in part, a function of short-chain fatty acids eliminated in feces. When we offer the body a menu of slower-digesting foods, the gut microbes break them down in the process known as fermentation, yielding short-chain fatty acids. These SCFAs improve metabolic health; indeed, gut ecosystems optimized for fermentative metabolism and higher bacterial growth rates appear to be conducive to weight loss.
Not All Calories are Created Equal
According to a study published in the journal Nature Communications, the human body appears to react differently to calories ingested from high-fiber whole foods vs. ultra-processed or “junk” foods. The latter get absorbed faster upon entering the upper GI tract, rendering fewer calories enter the gut microbiome at the end of the digestive tract. Conversely, high-fiber foods can remain intact longer, sustaining the full journey to the large intestine. Here, the trillions of bacteria comprising the gut microbiome can begin to get busy. Interestingly, the net result seems a reduction of caloric intake.
The study reveals that gut microbes exist in a perennial tug of war with the rest of the body for calories, said Karen D. Corbin, an investigator at the AdventHealth Translational Research Institute of Metabolism and Diabetes in Orlando and the lead author of the study. She further adds, “On a Western diet that doesn’t feed the microbes very much, almost all the energy goes to us and very little goes to the microbes. We don’t give the microbes any opportunity to utilize the calories we ate because we use them all. We pull the rope all the way to one end.”
To minimize early absorption and to maximize the quantity of food ultimately reaching the microbes in the large intestine, choosing a diet comprised of whole foods rather than their processed counterparts keeps the gut microflora happy and in peak working order. Such a meal plan advocates eating whole nuts over nut butter, steak instead of ground beef, and fresh whole fruits as opposed to processed juices to improve gut health and ultimately leads to weight and body fat loss, a primary reason clients state for seeking out the expertise of personal trainers.
The Gut Microbiome and Organ Cross-Talk
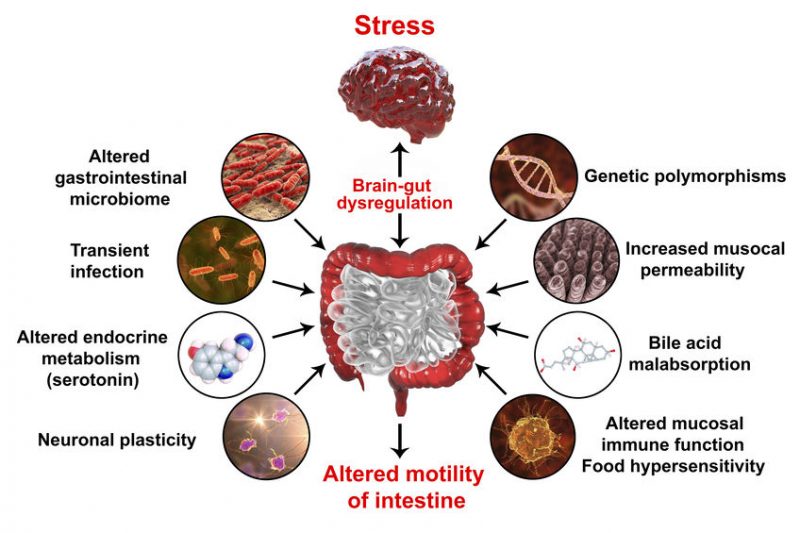
Upon closer inspection, scientists noted the presence of what they call “bi-directional cross-talk” between host microflora and the endocrine system, the point of origin for autoimmune dysfunction. The immune system participates in such cross-conversation.
The gut microbiome not only regulates systemic immunity; the immune system also contributes to the biodiversity of the microflora. This mutual communication between the microbiota and the immune system underscores how the human body’s health relies on “outside-in” and “inside-out” systems of checks and balances.
The ever-evolving studies on intestinal microflora now demonstrate that inflammation within the central nervous system also stems from our gut health. Once again, bi-directional communication occurs, referred to as the “brain axis signaling pathways”.
When gut health is prioritized, brain signals are transmitted through connections involving neurogenesis, neural transmission, and behavioral control. Disruption to the indigenous gut microbiota renders these pathways dysregulated; the resulting altered permeability negatively affects the blood-brain barrier. It seems feasible then to see how gut health has a powerful impact on mental health, most notably stress, depression, and anxiety disorders. As a prime example, over 20% of individuals living with chronic inflammatory bowel disease suffer from some manner of sleep disturbances and depression.
The “Inside-Outside” Scoop
Clients often open up to us about how they “do everything right” with regard to lifestyle and diet, yet still cannot achieve their goals. Educating them about the far-reaching effects of their gut microbiome could shed some light on their predicament. Trainers have the ability to guide clients, reminding them how healthy insides keep us fit and disease-free.
Tailoring A Mediterranean Plan to American Tastebuds
The microbiome-enhancing diet consists of foods that rank high in what scientists call “resistant starch”, including fresh fruits/vegetables, oats, beans, lentils, nuts, and whole grains. It extolls the virtues of meals based around whole, single-ingredient plant-sourced foods. Fresh and dried fruits, vegetables, legumes, whole grains, fresh fish, olive oil, and fermented dairy products comprise the backbone of this plan. Red meat, refined sugar, and processed foods rarely get consumed. Plenty of water and a daily glass of red wine figure prominently, along with reasonable amounts of physical activity and plenty of community socialization.
Clearly, one need not reside on the shores of the Mediterranean Sea to take advantage of this healthier eating style. We can find the majority of appropriate foods in grocery stores and farmer’s markets nationwide. This 3-day sample plan-at-a-glance might provide ideas and spark culinary creativity:
Monday
- Breakfast: Greek yogurt/strawberries /oats
- Lunch: Sandwich with vegetables/whole grain bread
- Dinner: Tuna salad with olive oil/piece of fruit
Tuesday
- Breakfast: Oatmeal /raisins
- Lunch: Leftover tuna salad
- Dinner: Salad of greens, tomatoes, olives, and feta cheese
Wednesday
- Breakfast: Omelet of spinach/tomatoes/onions; piece of fruit
- Lunch: Sandwich with cheese/fresh vegetables, whole grain bread
- Dinner: Broiled salmon/brown rice/vegetables
If hunger strikes between the 3 daily meals, choose healthy snack options:
- handful of nuts
- fruit
- carrots /hummus
- Greek yogurt
- apple slices /almond butter
Sean Gibbons, a microbiome specialist and assistant professor at the Institute for Systems Biology in Seattle, emphasized the results of this new study, highlighting how individuals could lose weight/body fat simply by switching to such a diet, potentially even in the absence of intense exercising or reducing calories. Gibbons went on to say that these results confirmed what he observed in his own research. Nutritionally encouraging growth and activity within our gut microflora yields positive metabolic health and thus desired weight loss.
Business Boost
The fact that so many personal trainers see an increasing number of seniors among their client base reflects this ever-growing population. We do our best to keep such clients functionally fit, to maintain or improve the quality of their older years. If a different approach to nutrition can also enhance their lives, trainers might consider educating their clients on the many benefits of shifting to a whole foods diet to support gut health. Lunch-and-learn seminars on the Mediterranean diet and longevity may help steer personal training businesses toward this age demographic.
[sc name=”nutrition-preview” ][/sc]
References:
healthline.com/nutrition/mediterranean-diet-meal-plan#foods-to-avoid
healthline.com/health-news/heres-what-to-eat-to-keep-your-gut-happy
ncbi.nlm.nih.gov/pmc/articles/PMC7306987/#R17ueg.eu/a/30
piedmonthealthcare.com/mediterranean-diet-a-recipe-for-strength-in-old-age/Fmercu
foodbusinessnews.net/articles/15501-mediterranean-diet-linked-to-healthy-aging
nutraingredients-usa.com/Article/2020/02/19/Mediterranean-diet-promotes-gut-bacteria-linked-to-healthy-aging-in-older-people-Study#
https://www.washingtonpost.com/wellness/2023/06/13/weight-loss-calories-fiber-microbiome/?pwapi_token=eyJ0eXAiOiJKV1QiLCJhbGciOiJIUzI1NiJ9.eyJzdWJpZCI6IjM5MjM2MjI5IiwicmVhc29uIjoiZ2lmdCIsIm5iZiI6MTY4NjYyODgwMCwiaXNzIjoic3Vic2NyaXB0aW9ucyIsImV4cCI6MTY4NzkyNDc5OSwiaWF0IjoxNjg2NjI4ODAwLCJqdGkiOiJiMWFiY2VlOC0xMDBkLTRjOTgtOGRlYi02MTU5MWU4NGRlNGMiLCJ1cmwiOiJodHRwczovL3d3dy53YXNoaW5ndG9ucG9zdC5jb20vd2VsbG5lc3MvMjAyMy8wNi8xMy93ZWlnaHQtbG9zcy1jYWxvcmllcy1maWJlci1taWNyb2Jpb21lLyJ9.86-vKnonCAZ0wQ7rdlQqa-iL2BerSnCvhPUSyRyeH0Q
https://www.nature.com/articles/s41467-023-38778-x
https://journals.asm.org/doi/10.1128/mSystems.00964-21
researchgate.net/publication/267456880_Crosstalk_between_intestinal_microbiota_adipose_tissue_and_skeletal_muscle_as_an_early_event_in_systemic_low_grade_inflammation_and_the_development_of_obesity_and_diabetes
pubmed.ncbi.nlm.nih.gov/28968517/
pubmed.ncbi.nlm.nih.gov/28675945/
ncbi.nlm.nih.gov/pmc/articles/PMC7510518/
ncbi.nlm.nih.gov/pmc/articles/PMC6104804/
atlasbiomed.com/blog/link-between-gut-bacteria-and-weight-loss/
pubmed.ncbi.nlm.nih.gov/31547555/
pubmed.ncbi.nlm.nih.gov/31451009/
pubmed.ncbi.nlm.nih.gov/31861086/
https://pubmed.ncbi.nlm.nih.gov/29861127/
https://pubmed.ncbi.nlm.nih.gov/26185088/
https://pubmed.ncbi.nlm.nih.gov/33362788/
https://www.washingtonpost.com/wellness/2023/06/13/weight-loss-calories-fiber-microbiome/
https://www.nature.com/articles/s41467-023-38778-x
Cathleen Kronemer is an NFPT CEC writer and a member of the NFPT Certification Council Board. Cathleen is an AFAA-Certified Group Exercise Instructor, NSCA-Certified Personal Trainer, ACE-Certified Health Coach, former competitive bodybuilder and freelance writer. She is employed at the Jewish Community Center in St. Louis, MO. Cathleen has been involved in the fitness industry for over three decades. Feel free to contact her at trainhard@kronemer.com. She welcomes your feedback and your comments!

