This just in: Teen bodies are going through changes! Perhaps not in the way you’d expect, though. A 2018 study has re-emerged, covered in the last weeks by the BBC, TIME magazine, and spanning the internet with a viral frenzy, discussing strange bony growths showing up on the back of teens’ heads resembling “horns”. Let’s dig into the deets and gain some perspective to share at the water cooler!
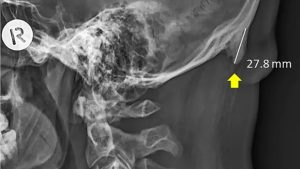
Shahar & Sayers (2018)
The Study Discovering “Horns”
Clinical researchers with the University of the Sunshine Coast in Queensland, Australia presented some interesting data in a 2018 paper: EEOP is not only a goofy acronym, but an underlying epidemic in our youth. While the internet has basically exploded with overreactions to the findings, attributing these strange occipital horns directly to cell phone use. As with any gripping story like this, we’re going to hear about it from our clients and patients, and it’s our responsibility as professionals to have intelligent and informed responses, if not rebuttals, to such things.
Here’s the gist:
EEOP in the paper stands for Enlarged External Occipital Protuberance. If we recall from anatomy, the EOP is the little shelf at the back of our skull. That first E should actually stand for Enthesopathic, because the enthesis in the subjects seems to be chronically irritated and calcified. Basically, the neck tendons attached to the base of the skull had begun to turn to bone.
Nearly 30% of the 18-30 year old group had horns that were not within normal limits…over 10mm and up to 30mm. These findings correlated almost perfectly with patients who had FHP (Forward Head Protraction), aka Anterior Head Carriage. Usually, EEOP is more commonly found the OLDER we get…but for some reason this grouping of young patients had a higher prevalence than their age 50+ counterparts. This ultimately led the researchers to conclude that increased hand-held tech usage was to blame.
The Real Problem Causing “Horns”
The study was very well done, accounting for age, gender, and being a good sample of a generally normal population with a sample size of over 1000 subjects. Additionally, only 50% of the younger group had reported musculoskeletal pain, while the other half was asymptomatic (pain-free), which helps rule out some other confounding factors. Despite being well-executed, Authors of the study make a few goofy suppositions that confound the ultimate message of the study.
- While rightly pointing out that previous generations have dealt with anterior head carriage issues, i.e. reading books, the use of hand-held devices is MUCH higher in modern society. As a fact, we deal with more postural strain at the neck than any previous generations because of access to current technology.
- The authors comment at their confusion on how the Achilles tendon receives similar strains but does not deform further like the EOP. This shouldn’t be confusing…the muscle attachments at the neck have to CONSTANTLY fight gravity to keep our 11 lb bowling ball of a head to not fall further forwards, while the Achilles doesn’t tug the heel against gravity, has a better lever-arm to reduce force needed, and is in or near neutral joint position most of the time.
- In the study, it is shown that females experience EEOP less than their male counterparts. Some literature suggests this is behavioral, commenting on how video-gaming and screen time is higher in males, thus the difference in findings. Other authors suggest differences in head weight, muscle strength and moment arm lengths, as well as more moderate synthesis in collagen in women versus men.
In addition to those factors, women tend to have a different distribution of tissue cells and hormones, and are thusly more flexible compared with the more hypertonic male tissue. The missing link here is that female neck muscles may be able to distribute the repetitive postural stress somewhat more easily while not irritating the occiput itself.
Ultimately, my personal take on it is this: Horns like this rarely happen for no reason, and certainly not in 33% the population. Humans may take 25 years on average to have fully formed bones. Inappropriate stresses during our formative years on the planet will tug and pull at bony structures, causing those structures to deform and reform to meet those stresses.
It’s why martial artists can punch through brick and ice. It’s why bunions form. This, these bony projections, is how bone heals when it’s tugged and smashed –one of the delights of our evolutionary advantage: we adapt.
Unfortunately for our generation, tech youth may be getting the raw end of the deal here due to completely controllable factors. The more we look down, the more stress on the neck muscles, and if our muscles aren’t up to the task, the stress goes straight to the attachment site. The younger we are, the less our system can handle that stress.
Then, boom: horns.
A Solution for Text Neck
Too bad Google Glass didn’t take off! That could be the solution here: Looking straight ahead instead of down. But perhaps that would have been the start of a whole other set of issues…hahah! But let’s say for the sake of argument that we’re going to invent a solution here as movement professionals.
Let’s say we call it “Rehabilitation for Ergonomic Stress in Teens“, or REST for short. How would YOU fix this supposed epidemic with your skill set? What would be your REST system? Here’s my answer:
-
Ergonomics
Before all else, this is the most conservative answer. Teaching or cueing proper posture in your clients is so important with how prevalent technological interaction is. Just do a checklist on yourself right now. Do you slouch and crane your neck when you drive? At work? Sitting at the computer? Looking at your phone? Watching Netflix on the couch? Reading in bed? The answer is simple. Get your body into an ergonomic position and fit the work to the worker. This means bring the phone a few inches higher, be eye level with your computer monitor, bring your seat forward in the car, etc.
-
Limit stressful positions
A less conservative intervention because we’re essentially removing activity, this is the next best thing to proper ergo. When patients of mine have overuse or repetitive stress injuries, sometimes we just need to find the right balance of activity that doesn’t overload the tissues AND still allows the tissue time to heal between stresses. Cut behaviors in half to start, and be observant of the outcomes. Just add or subtract as necessary! That’s one hour of gaming instead of two. Do-able!
-
Stretch and Exercise
A no-brainer, right? I was disappointed to see a complete lack of this suggestion in the paper. We all know that when one side of the joint is short and tight, the other is also pulled tight….right? When X contracts, the opposing muscle Y has to relax, but it also goes into a stretched position. What happens if X is all the way lengthened AND contracting? It’s essentially perpetually in an eccentric or isometric load with poor leverage.
A few ideas to help calm this musculoskeletal quandry:
-
- Chin Tucks (Deep Cervical Flexion)
Upper cervical retractions can strengthen the right areas while alleviating stress on the wrong ones. It’s helpful to lean the back of the head against a wall. Use a hand to press the chin in towards the neck while actively trying to make a “double chin”. The cervical extensors should be taut and stretching. Hold for 3-5 seconds and release. Repeat for 10 repetitions.
- Chin Tucks (Deep Cervical Flexion)
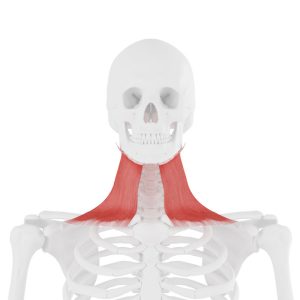
Platysma
-
- Platysma Stretch
This is your Arnold Schwarzenegger muscle. While your deep neck flexors may be hard to get at, this one is an easy one to find, and has the best mechanical advantage for keeping your head stuck in a forward position. Platysma is a relatively thin muscle, acting much like a mantle or cowl, dripping down our chin to our clavicles. I teach my patients and clients how to pin and stretch this muscle, as the deeper neck flexors are hard to target and the platysma has the best mechanical leverage for keeping the neck locked tight into a flexed position.
- Platysma Stretch
To “unlock” it, simply get into a flexed and tucked position with your neck, pinning your fingertips against your clavicles, and slowly drawing your nose and chin skyward as you feel the skin, fascia, and muscle tease its way out from under your fingers to stretch.



In conclusion, research can be misinterpreted and reinterpreted all day. This author suggests that in light of the obvious findings and knowing how the human body reacts to stress, we should take precautions to help ourselves and our clients by utilizing our unique skill set to offset the deleterious effects of poor postural patterns. Your homework? Say that 10 times fast.
References
Shahar, David; Sayers, Mark G. L. (2018). “Prominent exostosis projecting from the occipital squama more substantial and prevalent in young adult than older age groups,”. Scientific Reports, 8(1): 3354.
(www.nature.com/articles/s41598-018-21625-1)
www.bbc.com/future/story/20190610-how-modern-life-is-transforming-the-human-skeleton
www.drposture.com.au/2010/08/about-dr-posture/
www.erikdalton.com/blog/forward-head-posture/
www.time.com/5611036/teenagers-skull-horns/
Dr. Patrick K. Silva is a Board Certified and Licensed Doctor of Chiropractic with a focus on Sports Rehab, practicing in the beautiful US Pacific Northwest. Building on his preceptorship with the Seahawks' chiropractor (Dr. Jim Kurtz) in 2016, Dr. Patrick has designed his practice around the numerous soft tissue techniques, movement systems, and rehabilitative paradigms that modern sports science has to offer. Dr. Patrick is also a Certified Office Ergonomics Evaluator and Certified Professional Trainer. In his spare time, Dr. Patrick enjoys DIY projects and stays active practicing martial arts, soccer, dodgeball, parkour, and gaming.


